Imagine performing all your blood tests using a chip smaller than your palm, with just a drop of blood. Wouldn’t that make blood tests feel less daunting, more accessible, and far more comfortable? You might think this is the plot of a sci‑fi movie. But the surprising twist is, it’s real, and it’s happening right now in India.
Welcome to an era of healthcare powered by microfluidics.
Microfluidics may sound complex, but it simply involves manipulation of tiny volumes of fluid, measured in microlitres or nanolitres, within well-designed chips. It also finds many applications in various sectors of healthcare.
Advancements in designing and developing microfluidics devices have made it a reality to miniaturise conventional laboratories into an efficient and cost-effective microchannel tool. These devices function with a drop of blood, urine, or saliva and can be used for the diagnosis of multiple tests, within minutes, on the chips. These chips are usually etched or printed on materials like paper, glass or plastic, and control the transport of fluids to various compartments that are specific to the analyte to be tested (Kumar et. al, Songok et. al, Nielsen et.al, Smith et. al).
They eliminate the need for expensive and huge machinery and laboratories, and at times, the requirement of skilled personnel. It is rapid, portable, affordable, accessible, and precise. These devices are a combination of smart engineering with a dash of innovation.
Why should India care about microfluidics?
The Indian healthcare industry is valued at $ 98.98 billion in 2023 and is estimated to reach $193.59 billion by 2032. Although the healthcare system of the country is improving, it still remains under massive pressure due to the large rural population with limited access to diagnostic labs, long distances of travel, shortage of trained technicians, and overburdened urban hospital staff. Microfluidics becomes a game-changer for this scenario. A community health worker could simply carry a pocket-sized device to the rural areas and diagnose health issues such as tuberculosis (TB), dengue, malaria, and diabetes, right there, without the need to transport the samples to far-off labs.
Yes, this is the future that is already under trial at certain locations.
The quiet revolution of microfluidics is already underway in numerous laboratories, startups and universities across the country. Diagnosis of health issues such as TB, dengue, and malaria is being performed using microfluidics. Startups present portable tests that can deliver faster results without depending on heavy infrastructure. Rapid diagnostic test kits are also being developed for maternal and child health conditions like anaemia, gestational diabetes, and infections during pregnancy. These devices aid frontline health providers in screening women in a fast and safe manner in low-resource settings. Microfluidics also enables addressing the growing concern of lifestyle diseases such as diabetes, cardiovascular health, and thyroid disorders in the country. The majority of these health issues require continuous monitoring rather than a one-time test. Microfluidic devices enable continuous and low-cost monitoring at home or local health clinics and reduce the load on hospitals.
Numerous institutions and research laboratories have been working on the development of such innovative solutions. The recent award to Suman Chakraborty, Director, IIT, Kharagpur for developing affordable medical diagnostics is a testament to India’s homegrown innovators. A few homegrown innovators, such as Mylabs Discovery Solutions, Achira Labs, Module Innovations, SigTuple, and OmiX Labs are revolutionising the healthcare industry. Innovators are developing affordable microfluidics-based diagnostics for hormone levels, infections, and chronic conditions. Startups are also integrating AI for automating sample analysis in order to reduce dependency on skilled personnel. These key players are not just enabling the country to catch up, but rather leading in frugal and scalable healthcare solutions.
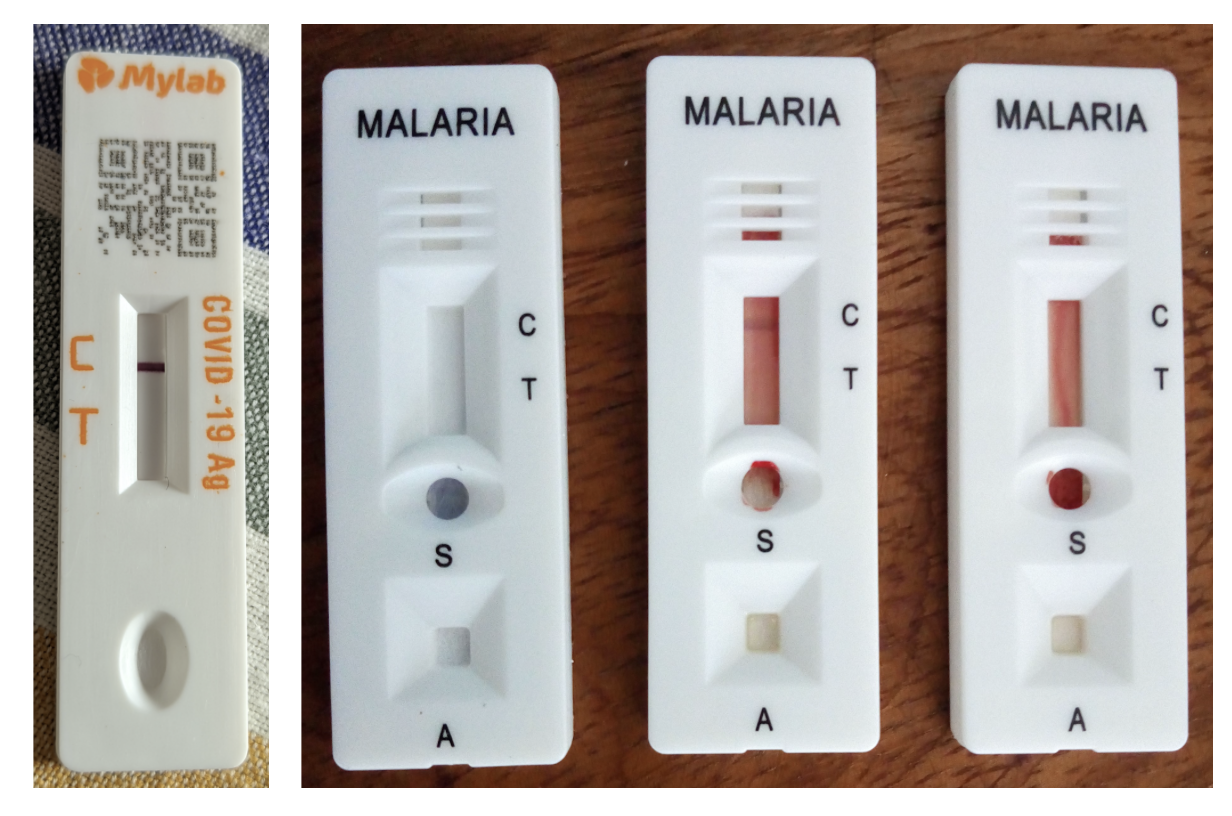
Few commercially available solutions. (COVID Self RAT, Malaria test kit)
Why now? Why are the researchers so focused now on microfluidics?
One of the major drivers behind this is the COVID-19 pandemic. The pandemic increased the demand for rapid, portable testing and microfluidics fit right into it.
The other factors driving this era are the growth of India’s startup ecosystem for biotech entrepreneurship, academic innovations in premier institutions like IITs, IISc, IISERs, CSIRs and NITs, that propel the research and aid incubating student-led innovations. The Indian government has also been extending numerous initiatives such as Make in India, BIRAC, and Startup India, funding as well as policy support, in order to promote such innovations.
In the journey of revolutionising healthcare with microfluidics, there have been innumerable challenges. Some have been addressed, whereas others still have a long way to go. Even though these solutions are cheaper than the laboratory tests per use, the development and manufacturing of these devices at a large scale still remains costly for the Indian market. Not all materials, prototyping tools and skilled personnel are readily available domestically. Another major challenge lies with the regulatory approval process from authorities. The process is time-consuming, complex, and at times exhaustive. Quite a number of innovators end up struggling to move ahead from this stage. Another factor to account for is that the device is only as good as the user. The Indian healthcare system needs training modules for frontline workers to enable them to use and trust microfluidic tests. And in order for these tests to reach the rural and low-resource settings, devices require local manufacture, reliable distribution and easy maintenance, all of which are still a work in progress.
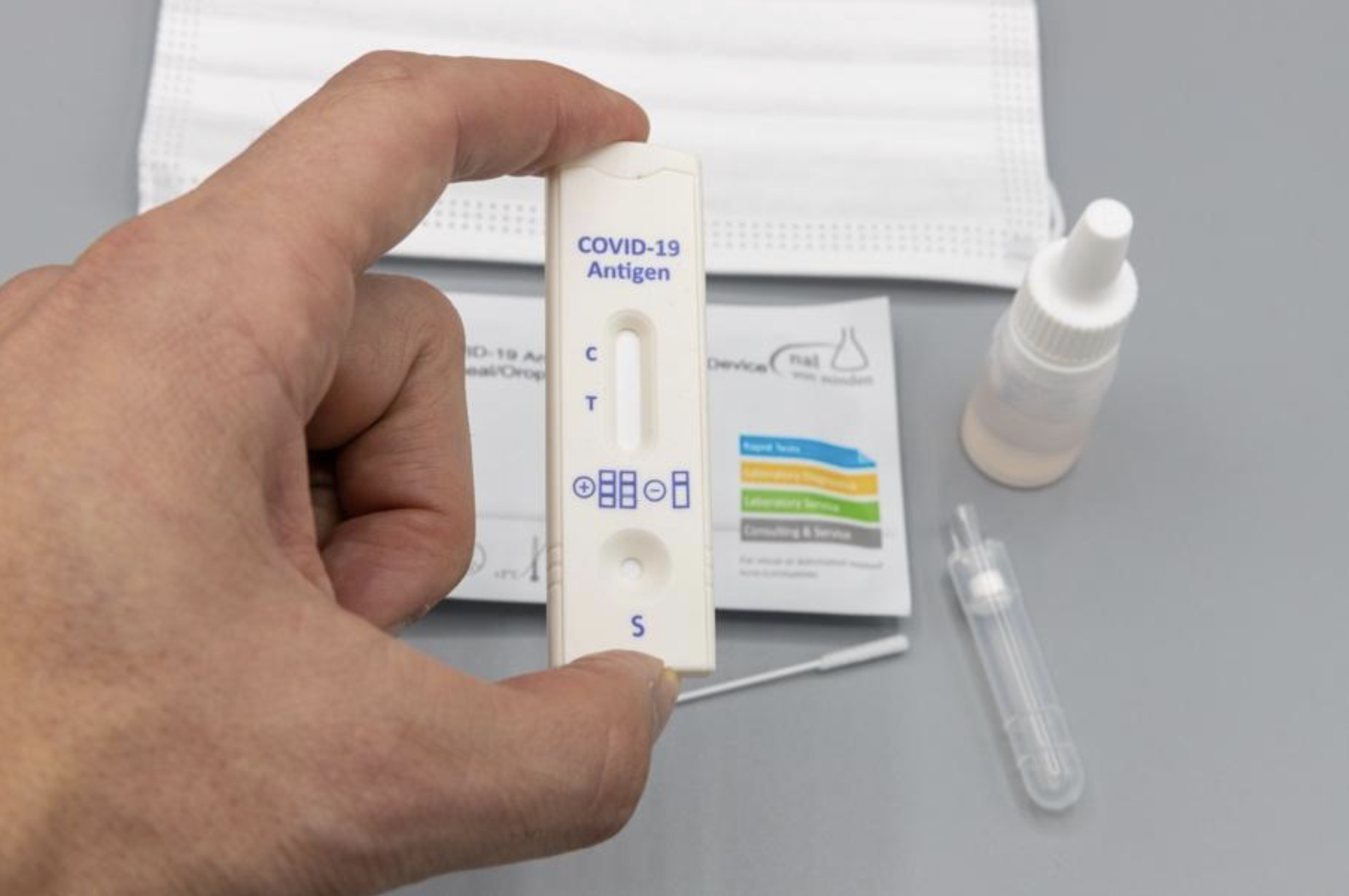
RDT (Rapid Diagnostics Test) tests are used in healthcare facilities for COVID, a post COVID effect, for faster diagnostics. (COVID antigen rapid test)
So, what’s the opportunity?
Despite these challenges, the potential of microfluidics in healthcare still remains massive. India has the patient volume, disease diversity and talent pool in order to benefit from this technology and lead its development on a global stage. This potential would enable an Asha (Accredited Social Health Activist) worker to perform their primary roles in their communities, such as raising awareness about health issues, facilitating access to health services such as maternal and child care, and mobilizing the community for improved health outcomes. These trained female community health activists in India may use these devices to diagnose malaria on the spot, enable a school health checkup to screen for health issues instantly and help patients monitor their health issues at home. For India to truly harness the power of microfluidics, academia needs to facilitate interdisciplinary education across fields. A new curriculum should be designed that merges biology, engineering, design, and entrepreneurship for university-level courses. There is also a need for increased funding support in terms of grants and seed money for healthcare innovations. Startups also require support for connections to suitable government healthcare systems for increased field trials. Domestic production of the components for the development of such devices needs to be highly incentivised. Researchers should be encouraged to share designs, results, and best practices for collaborative facilitation of microfluidic healthcare innovations.
One must understand that microfluidics is not a replacement for healthcare providers or institutions. It is a revolution to bring the diagnostics closer to the common population, and the ones that need them the most, especially in remote and low-resource settings, such as villages, slums, small towns, as well as crowded clinics. This revolution is quiet, yet already on the way. The next huge leap for Indian public health might not be from a massive hospital chain or a fancier global deal. It would be from a tiny chip, powered by homegrown science, and delivered by a local health worker, to save lives. One test at a time.